Collateral Blood Flow
 Collateral vessels can play a significant role in supplying oxygen to a tissue, particularly when oxygen delivery is limited by disease in the normal vasculature. Collateral vessels are pre-existing vessels (usually small arteries and arterioles) and their blood flow depends on the distribution of pressures within the vascular bed as well as on their vascular resistance. They are secondary supply vessels in terms of their perfusion of a tissue region. Acute occlusion (e.g., thrombosis) of a primary supply artery can cause a redistribution of pressures within the vascular network that cause increased flow to occur in pre-existing collateral vessels.
Collateral vessels can play a significant role in supplying oxygen to a tissue, particularly when oxygen delivery is limited by disease in the normal vasculature. Collateral vessels are pre-existing vessels (usually small arteries and arterioles) and their blood flow depends on the distribution of pressures within the vascular bed as well as on their vascular resistance. They are secondary supply vessels in terms of their perfusion of a tissue region. Acute occlusion (e.g., thrombosis) of a primary supply artery can cause a redistribution of pressures within the vascular network that cause increased flow to occur in pre-existing collateral vessels.
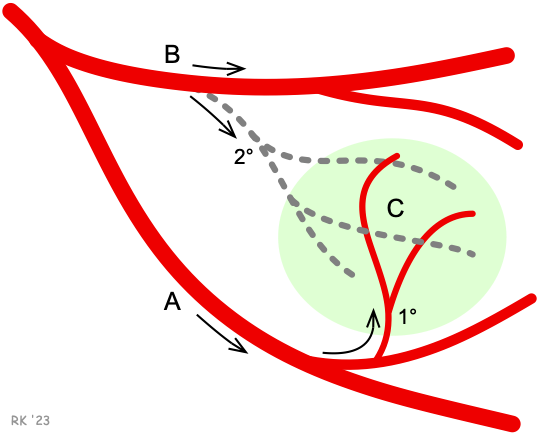
These principles are illustrated in the figure. A region of tissue (C; green highlight) is supplied primarily by artery A; however, there is a secondary, collateral circulation (dashed lines) supplied by artery B. If artery A were to become occluded, then flow to the tissue region would cease if artery A were the only arterial supply. However, because of the secondary collateral supply, flow to the tissue may still be partially maintained by flow derived from artery B. Because the tissue initially becomes ischemic because of the loss of its primary supply, the collateral vessels can respond by dilating (metabolic vasodilation), which will increase their blood flow to the tissue.
Collateral blood vessels are important in skeletal muscle and coronary circulations. Conditions of chronic limb ischemia, caused by arterial disease, for example, can lead to increased development of collateral vessels. These vessels are in parallel with the diseased vessels and therefore can partially take over the function of supplying blood flow to the limb. These collateral vessels, along with flow autoregulation, can help to maintain adequate blood flow in the resting limb despite narrowed, diseased vessels. However, maximal flow capacity is ordinarily reduced despite the collaterals. In the heart, collateral vessels can help to supply blood flow to ischemic regions caused by stenosis or occlusion of epicardial arteries. Collateral blood flow is an important mechanism helping to limit infarct size in the heart when a large coronary artery suddenly becomes occluded by a thrombus. Endurance exercise training promotes the growth of new microcirculatory vessels by the process of angiogenesis, which improves vessel collateralization within organs such as the heart. There is ongoing research to stimulate the formation of collateral blood vessels by treating the heart with drugs that stimulate angiogenesis.
Revised 11/03/2023

 Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021)
Cardiovascular Physiology Concepts, 3rd edition textbook, Published by Wolters Kluwer (2021) Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)
Normal and Abnormal Blood Pressure, published by Richard E. Klabunde (2013)